Support Client Access to Healthcare Practitioners
Cochrane District Services Board: Pilot Project to Support Client Access to Healthcare Practitioners
Addressing Health Barriers for Long-Term Social Assistance Clients
By: Christine Heavens
April 2025
In 2023, the Cochrane District Services Board (CDSB) undertook a comprehensive analysis of its client demographic, revealing that 25% of its caseload had been on social assistance for five years or more. This deep dive into the reasons for the prolonged need for social assistance identified significant health barriers, including physical impairments, mental illnesses, and addiction issues, which impede clients' success.
The data further showed that 57% of the clients on social assistance for more than five years may not have access to a healthcare practitioner. To address these challenges, CDSB launched a pilot project in 2024 aimed at enhancing client access to healthcare practitioners.
Ontarians have been aware of the doctor shortages for years. In fact, the Ontario College of Family Physicians share that by 2026, 1 in 4 Ontarians will be without a family doctor. Considering that the Cochrane District’s clients have already reached this statistic, it is likely that social assistance clients are, and will continue to be, disproportionately affected.
Importance of Access to Healthcare Practitioners
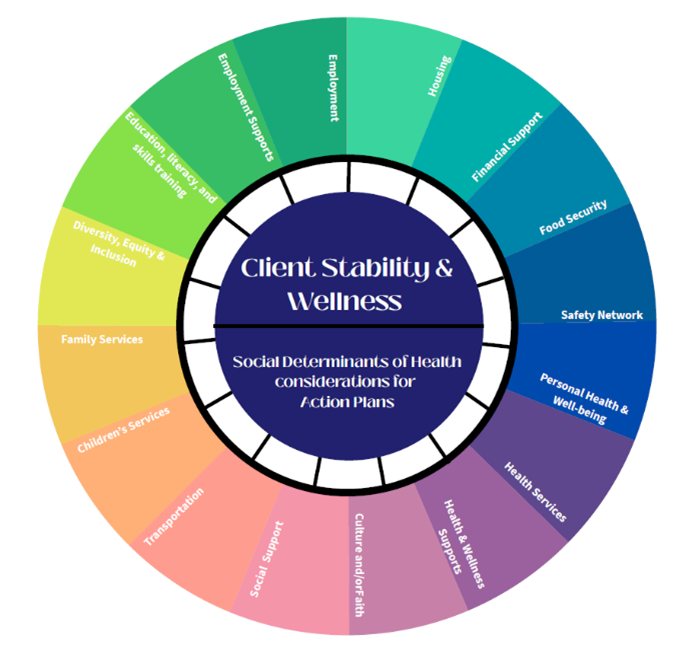
The impact of this service gap puts a client's health outcomes at risk. Consider the social determinants of health, including their:
- Housing stability: placing people at a higher risk of homelessness. Between August 2023 and August 2024, the Cochrane District experienced a 39% increase in homelessness, with the number of people affected rising from 293 to 407.
- Food security: At the time, Stats Can reported that food costs alone had risen by 5.9% in 12 months.
- Mental Health: Financial pressures and a lack of financial stability negatively impact the client’s mental health, making life stabilization difficult (if not impossible).
CDSB's Pilot Project
CDSB recognized the need to address systemic health barriers and conducted an inventory of available health resources available to clients in the district. This led to securing a private nurse practitioner in Iroquois Falls. The pilot project aimed to support:
- Assessment and each client’s health prognosis.
- Development of a plan for return to work and/or
- Completion of the necessary documentation to apply to the ODSP program.
Although assigned OHIP billing numbers, Nurse Practitioners (NPs) cannot bill OHIP directly on a fee-for-service basis. Thus, CDSB needed funding to support the NP's work. A three-way partnership was secured involving the Canadian Mental Health Association, who provided financial support for the project. The collaboration was captured through a Memorandum of Agreement.
Project Results

The average number of NP visits per client was two, with the first visit for assessment and test ordering, and the second for reviewing results and outlining the health plan. Three clients were redirected back to employment through health pathways.
A snapshot of the quantitative results included:
- 58% of clients served were aged 30-49
- 75% were single, and 19% were families
- 54% identified as Caucasian, and 36% as Indigenous
- 42% had mental health or addiction issues, and 33% had physical restrictions
DAU Decision
Over a seven-month period, 53% of the clients who were supported with an ODSP application were granted. Of these, 28% were Indigenous, 78% required no review, 16% required a two-year review, and 6% required a five-year review. However, 47% of applications were denied.
Clients with denied applications were encouraged to appeal, with support provided through referrals to local legal clinics. However, despite the offer of support, some clients did not proceed with appeals, largely due to their deteriorating or all-consuming health conditions.
Testimonials
Client Testimonials
One client shared:
"I am grateful and happy I was finally granted. It has been a huge struggle, especially over the past two years. I am homeless and my next thing is to secure a residence since I will be getting more money. This will help me get custody of my children as I will have a better income. Thank you to all the OW [Ontario Works] staff for always being there for me when I needed them."
Another client expressed:
"I’m overjoyed that I can now afford to live!"
"Being on OW and unable to work, with no family doctor or family to help; this opportunity gave me HOPE. Now I can afford to eat and pay my rent!"
And finally, the gratitude from clients included:
"I’m in shock and don’t quite believe it. This is good news, thank you. Thank you for everything you have done to help me during my struggles.”
Case Manager Testimonials
Staff testimonials on the pilot include:
"I witnessed clients who were so overjoyed that they qualify for a special diet that they burst into tears."
When we received the news that our client had been granted ODSP, we cried, as we had worked with this client for over 10 years. This is truly a good news story."
"Through this process, I developed a more trusting relationship with clients, and it opened my eyes to many of the barriers beyond financials that many OW clients face."
Another case manager emphasized the importance of medical professionals on the team, stating, "When I received notice that my client was granted ODSP, ecstatic was not a strong enough word to describe how happy I was for her, knowing how long she struggled. It was a process, but it was successful. Having a medical professional on our team can improve the lives of so many of our clients. If we work together, we can achieve anything."
Next Steps
Not only does CDSB still have work to do to help clients access healthcare practitioners, but 47% of clients who got the help, which resulted in an ODSP application, were denied. These clients require ongoing commitment, support, and advocacy.
CDSB continues to engage with other healthcare practitioners across the district to secure continued healthcare spots and support for their clients. Hidden areas of support to date include Indigenous and French-focused healthcare providers. The plan is to expand partnerships to enhance access to health practitioners and continue monitoring and tracking data. CDSB also aim to collaborate with legal clinics and community partners, seeking ways to enhance submissions for better results while also advocating for the removal of red tape, so that social assistance teams can help clients access the financial and health services they need. Further project enhancements include the incorporation of client and partner feedback mechanisms to support process improvements.
About the Author

Christine Heavens, MBA, CET
Director, Community Development and Services
Cochrane District Services Board
As the Director of Community Development and Services, Christine Heavens excels at conceptualizing, articulating, and executing solutions to address complex, multifaceted regional and community issues through culturally inclusive and person-centred approaches supported by strong community partnerships. With 25 years of management and leadership experience in the public sector—over half of which as a senior corporate leader —Christine’s innovative approaches and collaborative efforts to address systemic barriers have earned her considerable respect within the Cochrane district and across the province. Ms. Heavens is an active member of the Boreal SSM consortium and executive team, serving as co-chair of the Far Northeast Training Board, chair of the District School Board of Ontario Northeast Special Education Advisory Committee, and a member of multiple other committees both regionally and provincially.
Christine possesses a Master of Business Administration (MBA) with a concentration in global leadership. She is accredited as a Certified Engineering Technologist and a Survey Technician. Additionally, by June, Christine will complete a Master's in Education, specializing in leadership in learning.
Special thanks to Blog contributors and Pilot Project Leads:
Tammy Smith, Ontario Works Program Manager
Chris Lachance, Ontario Works/ Housing Interim Program Manager
Please direct questions to Christine.heavens@cdsb.care
Blog categories: Ontario Works, Health, ODSP, Nurse Practitioners, Cochrane District Services Board